Simulation of Reflectance in Oral Tissue Using MCMatlab
Introduction
Clinical Motivation
Problem Statement
Background
Previous Work
Optical Tissue Properties in the Literature
| Tissue Layer | μa [cm⁻¹] 420 nm | μs [cm⁻¹] 420 nm | μa [cm⁻¹] 450 nm | μs [cm⁻¹] 450 nm |
|---|---|---|---|---|
| Superficial epithelium | 3.0 | 170 (keratinized) / 55 (non keratinized) | 2.1 | 140 (keratinized) / 40 (non keratinized) |
| Intermediate epithelium | 3.0 | 55 | 2.1 | 40 |
| Basal epithelium | 3.0 | 55 | 2.1 | 40 |
| Superficial stroma | 6.22 | 267 | 3.11 | 248.5 |
| Deep stroma | 6.22 | 267 | 3.11 | 248.5 |
| Blood | 262 | 37.8 | 30 | 31.1 |
Methods
Monte Carlo Simulation Principle
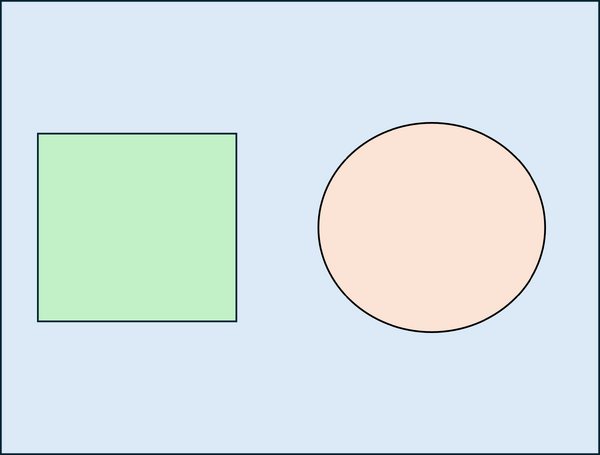
A simple Monte Carlo simulation can be used to estimate the value of π by comparing areas of a circle and a square. First, the geometric domain is defined, consisting of a square whose side is equal to twice the radius of the circle, so that the circle is fully inscribed within the square (see Figure 1a). A large number of points are then generated randomly and uniformly within the square. Each point is classified according to whether it lies inside the circle or outside, and the number of points falling within the circle is counted (see Figure 1b). The ratio of the number of points inside the circle to the total number of points in the square approaches the ratio of the areas of the circle and the square: . Multiplying this ratio by four therefore provides an estimate of π. This example illustrates how probabilistic sampling can be used to approximate geometric quantities.
|

|
| (a) Definition of the geometric domain | (b) Random point generation, classification, and counting |
| Figure 1: Basic Monte Carlo simulation to compute π | |
Monte Carlo Simulation for Light Propagation
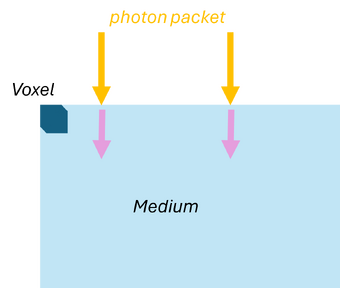
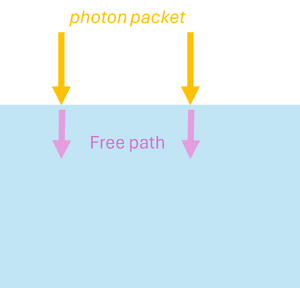
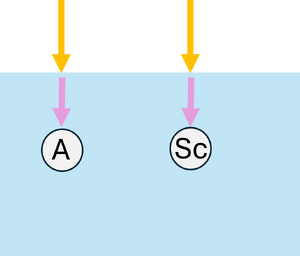
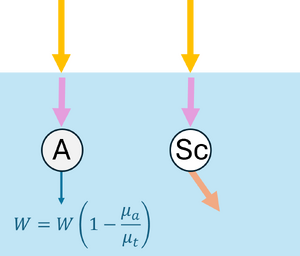
Monte Carlo simulations can also be applied to model the propagation of light in scattering and absorbing media, such as biological tissue. First, the geometric domain is defined, specifying the optical properties of the medium and the spatial grid where energy deposition will be recorded. A photon packet is then launched from the source with an initial weight (see Figure 2a). The photon propagates in a straight line over a free path drawn from an exponential distribution, , where (see Figure 2b). Upon reaching the end of the free path, an interaction occurs: the photon can be absorbed or scattered according to probabilities and . If scattering occurs, the anisotropy factor determines the preferential forward direction of the photon (see Figure 2c). During absorption events, the absorbed energy is and the photon weight is updated to , with the remaining weight continuing to propagate (see Figure 2d). By repeating these steps for many photon packets, the simulation statistically reconstructs macroscopic quantities such as fluence, reflectance, and transmittance in the medium.
|
|
|
|
| (a) Launching a photon packet | (b) Straight-line propagation over a free path | (c) Interaction event | (d) Updating the Photon Weight |
| Figure 2: Monte Carlo simulation for light | |||
Monte Carlo Matlab
Five Layer Model and Geometry
Results
Influence of Keratin on the Optical Response
Theoretical Results: Fluence
Note that all graphs are presented with arbitrary units because the Monte Carlo simulations are based on photon weights W, which do not give the exact number of photons. The fluence is defined as , where wi is the weight of photon packet i, μa is the absorption coefficient of the medium traversed, and δsi is the straight-line path length of photon packet i. Fluence can be interpreted as the energy density inside the tissue (i.e., how much light is present at depth z).

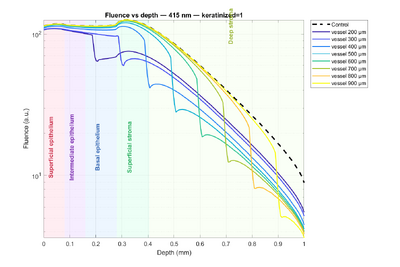
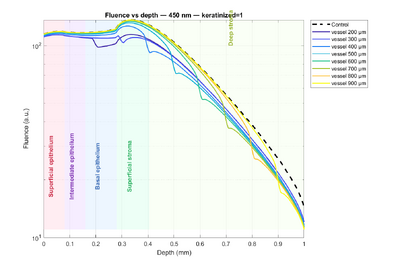
Let’s first focus on the impact of keratin in the tissue by looking at Figure 3 (dashed lines = non-keratinized tissue, solid lines = keratinized tissue). Two main differences are observed: first, in tissue with keratin, there is a small fluence bump in the superficial epithelium. Indeed, 170 (keratinized) / 55 (non-keratinized) at 451 nm and 140 (keratinized) / 40 (non-keratinized) at 450 nm, so there is a higher probability of light being scattered rather than absorbed → “more light” → higher fluence. Second, starting from the second layer, i.e., the intermediate epithelium, the trend reverses. Fluence is slightly higher in non-keratinized tissue. Interpretation: in keratinized tissue, light is “trapped” in the superficial epithelium due to strong scattering, so less light reaches the next layer.
Now let’s focus on the influence of wavelength. The difference between 415 and 450 nm shows higher fluence at 450 nm. Why? Because absorption is lower (smaller absorption coefficients). Finally, one key feature is the large bump between the epithelium and the stroma for all four curves. Since μa is doubled, fluence increases according to the formula above. All curves then decrease with depth due to absorption.
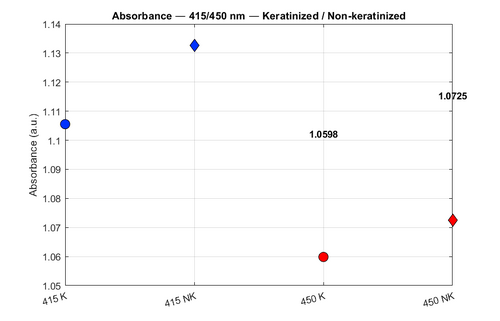
Measurable Results: Absorbance and Reflectance
Influence of Blood Depth on the Optical Response
Theoretical Results: Fluence
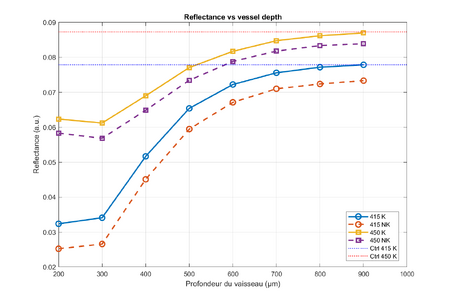
Measurable Results: Absorbance and Reflectance
Discussion and Conclusions
Appendix
Our code can be found at (Github link).